Careful planning of all technical components of augmentation mammoplasty is essential to ensure the best possible outcome. Implant size and shape selection are two of the most important components of this planning. There have been many descriptions of implant size selection.1-7 However, little is mentioned in the literature concerning a patient’s desired breast shape after augmentation.
With a new assortment of breast implants from low profile to high profile, plastic surgeons have more control as to the outcome of breast shape with breast augmentation. This is a simple classification of breast shape to help improve communication and set realistic expectations for breast augmentation results.
METHODS
During initial breast consultations, I felt that there had to be a better way to communicate with patients about their goals for postoperative breast shape than by utilizing pictures from lay media.
Often, a patient would state that they wanted a “natural” look but would show pictures with very round breasts. Because of these situations, what is needed is a more objective system to communicate patients’ aesthetic goals and obtainable results after breast augmentation.
A breast shape classification has been created in an effort to improve communication with patients and to achieve the best possible result based on that particular patient’s aesthetic desires.
This classification was used in the initial consultations of 30 patients. Preoperatively, patients were shown the breast shape classification with preop and postop pictures of other patients in each class on a screen. For example, if a patient desired a medium “C” with a class 3 breast shape, then they were shown pictures on the screen matching those wishes.

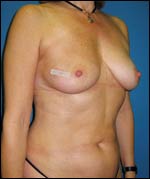
Figure 1: An example of class 1 breast shape. A 32-year-old with 32 B cup size breasts desiring a medium C with 1/5 in definition. Allergan Style 15 (moderate profile), 265-cc smooth round silicone implants were placed in a submuscular pocket in this 5-foot-6-inch, 120-pound patient.

Figure 2: An example of class 2 breast shape. A 25-year-old with 32 A cup size breasts desiring a medium C with 2/5 in definition. Allergan style 20 (moderately high), 260-cc smooth round silicone implants were placed in a submuscular pocket in this 5-foot-2-inch, 110-pound patient.

Figure 3: An example of class 3 breast shape. A 39-year-old with 32 A/B cup size breasts desiring a medium C with 3/5 in definition. Allergan Style 20 (moderately high), 325-cc smooth round silicone implants were placed in a submuscular pocket in this 5-foot-2-inch, 112-pound patient.
They were shown multiple before-and-after photos of patients with a similar body habitus and desires. They were then asked to rate their likes and dislikes in each photo. Using this method, patients provided more valuable insight into their desires in order to help their physicians achieve an improved result.
In our conversations to determine breast shape, the “volume” of an implant is not used. Instead, gauge the amount of preoperative breast tissue and the different profiles of implants available. For example, a class 4 or 5 breast shape would require a higher-profile implant to achieve a rounder appearance than a more natural-appearing breast, such as a class 2 or 3.
The size of implants chosen is then judged based on desired breast size (ie, small “C,” medium “C,” and large “C”) and the amount of breast tissue a patient has preoperatively. For example, a patient with B cup size breasts desiring a “large C” would probably get 300-cc implants, but a patient with A cup size breasts would more likely require 360-cc implants.
Intraoperatively, various sizers are used. The patient is placed in a sitting position to judge for final shape and size.
A survey was conducted postoperatively, with a mean follow-up time of 8 months (with a range of 6 months to 1 year).
RESULTS
These patients found the classification to be extremely helpful during the initial consultation. The classification was rated 9.3 out of 10 (with 1 being least helpful and 10 being most helpful) for communicating desires and developing realistic expectations. The correlation between preoperative and postoperative goals was rated as 9.2 out of 10 (with 1 being not close to 10 being extremely close).
DISCUSSION
Plastic surgeons have never before had a more complete assortment of styles of breast implants, which translates into greater control over breast shape.
An effective communication between the surgeon and patient regarding the size and shape after breast augmentation improves outcomes in terms of patient satisfaction. Sizing of the breast has been described in multiple previous articles and is beyond the scope of this article.8-15 Determination of shape is mentioned infrequently or not at all.
By using this new breast shape classification and teaching it to prospective patients, you have a very powerful tool in communicating shape issues with patients who often don’t have a good construct for knowing exactly what they want their breasts to look like after surgery.
When patients pick out pictures of breasts that they like, it is easy to assign a numerical value to the roundness of the breast from 1 to 5, and then make them aware of the type of breast shape that they like. This is more useful to determine shape than using preoperative sizers in a bra during consultation, as this technique can give inaccurate information and does not address the shape.
In the consultation, the final statement might sound like, “Mrs Smith, the breast that you desire would be a medium ‘C’ with 3 out of 5 in definition or roundness.”
This classification is helpful not only for communicating a desired breast shape between patient and surgeon, but also for setting limitations of a patient’s desire when their anatomy is not suitable for a certain shape.
For example, a patient with small breasts and minimal parenchyma will not be able to achieve a natural-appearing breast shape class 1. In this case, we would tell the patient that because she has little to no breast tissue, the best we can do is a class 2 or 3 in definition.
In contrast, a patient with fuller breasts and moderate parenchyma desiring a class 5-appearing breast shape would be difficult to accommodate because the moderate amount of breast tissue would cover the implant precluding the rounder, “unnatural” shape. In this situation, the patient would be told that this result would not be possible with breast augmentation alone, and a mastopexy might be recommended to achieve what she desires.

Figure 4: An example of class 4 breast shape. A 25-year-old with 32 A cup size breasts desiring a small C with 4/5 in definition. Mentor high-projection smooth round saline implants 330 cc filled to 330 cc were placed in a submuscular pocket in this 5-foot-5-inch, 110-pound patient.

Figure 5: An example of class 5 breast shape. A 29-year-old with 32 A cup size breasts desiring a large C with 5/5 in definition. Allergan Style 45 (highest profile), 360-cc smooth round silicone implants were placed in a submuscular pocket in this 5-foot-6-inch, 115-pound patient.
The use of a new breast shape classification has helped me communicate better with patients undergoing breast augmentation regarding their desired shape. In addition, it has been an extremely helpful tool during the initial consultation in setting realistic expectations, as well as pointing out limitations.
Paul E. Chasan, MD, FACS, is a plastic surgeon in private practice in Del Mar, Calif. He can be reached at (858) 450-1555.
The author acknowledges the contribution to this article by Karl Nguyen, MD.
References
- Mentor Corp. Saline-Filled Breast Implant Surgery: Making an Informed Decision. Santa Barbara: Mentor Corp, 2000;11-19.
- McGhan Medical Corp. Saline-Filled Breast Implant Surgery: Making an Informed Decision. Santa Barbara: McGhan Medical Corp; 2000: 10-18.
- Tebbetts JB. Dimensional Augmentation Mammaplasty Using the BioDimensional System. Santa Barbara: McGhan Medical Corp; 1994: 1-90.
- Tebbetts JB. Dual plane breast augmentation: Optimizing implant-soft tissue relationships in a wide range of breast types. Plast Reconstr Surg. 2001;107:1255.
- Gorney M. Preventing litigation in breast augmentation. Clin Plast Surg. 2001;28:607.
- Tebbetts JB. Achieving a predictable 24-hour return to normal activities following breast augmentation: Refining practices using motion and time study principles. Part I. Plast Reconstr Surg. 2002;109:273.
- Tebbetts JB. Achieving a predictable 24-hour return to normal activities following breast augmentation: Patient preparation, refined surgical techniques and instrumentation. Part II. Plast Reconstr Surg. 2002;109:293.
- Lipton B. Are you wearing the wrong size bra? Ladies’ Home Journal. March 1996;46.
- Young VL. The efficacy of breast augmentation: Breast size increase, patient satisfaction, and psychological effects (Letter) (Reply). Plast Reconstr Surg. 1995;96:1237.
- Thomas D. The quest for the perfect bra. SELF. March 1995;146.
- Penn J. Breast reduction. Br J Plast Surg. 1955;7:357.
- Yalom M. A History of the Breast. New York: Knopf; 1997: 172-183.
- Gittelson B. inventor; Triumph-Universa GmbH, assignee. Bust measuring device. US Patent 2 946 125. July 26, 1960.
- Smith DJ, Palin WE, Katch VL, Bennett JE. Breast volume and anthropomorphic measurements: Normal values. Plast Reconstr Surg. 1996;78:331.
- Westreich M. Anthropomorphic breast measurement protocol and results in 50 women with aesthetically perfect breasts and clinical application. Plast Reconstr Surg. 1997;100:468.
- Bouman FG. Volumetric measurement of the human breast and breast tissue before and during mammaplasty. Br J Plast Surg. 1970;23:263.
- Grossman AJ, Roudner LA. A simple means for accurate breast volume determination. Plast Reconstr Surg. 1980;66:851.