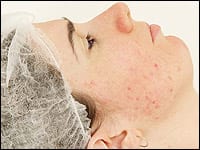
Finding a Cure for Rosacea
 |
Acne rosacea—also called adult acne—is an inflammatory skin disease that affects about 14 million Americans between the ages of 30 and 60. It is more common in women than in men, and it is more likely to affect fair-skinned people of European or Celtic descent.
Unlike acne, rosacea is not associated with a bacterial skin infection. Instead, it is characterized by facial redness (erythema) in areas that may include the forehead, nose, cheeks, and chin; by bumps and pimples (papulopustules), also called inflammatory rosacea; and by spider veins (telangiectasias), which occur when blood vessels under the skin of the face dilate, showing through the skin as small red lines.
Rosacea triggers include activities that cause the face to become flushed, such as exercise, stress, sunburn, sudden changes in temperature, alcohol, hot caffeine drinks, spicy foods, and even by blushing with embarrassment. The condition is chronic and gets worse over time. It is cyclical and flares up for weeks and months and then subsides.
Currently, there is no effective treatment for the skin disease. Antibiotics are sometimes prescribed, but they provide mixed results.
Researchers in the United States, France, and Japan, led by Richard L. Gallo, Md, PhD, professor of medicine and chief of the division of dermatology at the University of California, San Diego (UCSD) School of Medicine and the dermatology section of the Veterans Affairs San Diego Healthcare System, may have found the causes of acne rosacea.
In their study, published August 5 in the online edition of Nature Medicine, the scientists noticed that patients with rosacea had high levels of the antimicrobial peptide cathelicidin in their skin, which they believe caused the redness, bumps, pimples, and spider veins. They also noted that patients who did not have rosacea had the normal amount of the peptide in their skin.
The researchers also found that patients with rosacea had high levels of stratum corneum tryptic enzyme (SCTE), which converts cathelicidin into peptides that cause rosacea.
To test their theory, Gallo and his colleagues injected laboratory mice with the cathelicidin peptides found in rosacea, added SCTE, and increased the mice’s protease activity by switching off the protease inhibitor gene Spink5. The researchers noted that each of these actions increased inflammation of the skin.
 |
| See also “Skin Management: A Practical Approach” by Lawrence S. Moy, MD, with Catherine Maley, MBA, in the January 2007 issue of PSP. |
They also tested the role that cathelicidin plays in inflammation of the skin caused by SCTE by deleting the Camp gene.
“Too much SCTE and too much cathelicidin leads to the abnormal peptides that cause the symptoms of this disease,” according to Gallo. He also explained why antibiotics sometimes work in treating rosacea, even though the condition is not caused by bacteria.
“Antibiotics tend to alleviate the symptoms of rosacea in patients because some of them work to inhibit these enzymes. Our findings may modify the therapeutic approach to treating rosacea, since bacteria aren’t the right target.”
“These findings will play a critical role in finding more effective treatments for rosacea,” says David J. Goldberg, MD, JD, a dermatologist who practices in New York City. “Researchers, now understanding the true cause of rosacea, will be able to develop better and more specific treatments for this chronic, progressively worsening, skin condition.”
Reanimating Paralyzed Faces
According to a report in the July/August issue of Archives of Facial Plastic Surgery, a surgical technique called temporalis tendon transfer—in conjunction with intense physical therapy before and after surgery—may help reanimate the features of patients with facial paralysis.
 |
“The procedure will likely be a good alternative to traditional temporalis transfer,” says Babak Azizzadeh, MD, FACS, a facial plastic surgeon in Beverly Hills, Calif (see our cover story “Function and Form“). “I think that this is a significant and innovative advance in facial reanimation.”
Patrick J. Byrne, MD, the lead author of the study, and his colleagues at the Johns Hopkins University School of Medicine in Baltimore, reported the results of seven facial paralysis patients who were treated with temporalis tendon transfer.
According to the researchers, the technique, which addresses the inability to smile as well as an asymmetry in the lower half of the face, involves an incision that begins at the ear and ends 3 to 4 cm into the hairline at the temple. The temporalis muscle, a fan-shaped muscle on the side of the head, is cut at the point that it connects to the jawbone and is released from the tissue that is surrounding it. Then, it is stretched to the point where the muscles of the mouth join together.
The tendon that previously connected the temporalis muscle to the jawbone is cut free and stretched horizontally for 3 to 4 cm. It is then sutured to the surrounding muscles and to the deep skin tissue. Physical therapy to retrain facial muscles begins before the surgery and continues 7 days after the procedure.
Previously, surgeons used a different portion of the same muscle to try to restore function, a procedure that left the patient with some function but also facial deformity.
“The way it was done produced a depression or cavity in the temple region and a large protrusion around the upper cheek,” Byrne says. “Furthermore, the transplanted muscle itself has trouble moving well because if its unnatural position.”
The researchers note that 4 months postsurgery, patient satisfaction was very high. Of a possible 10 points, patient satisfaction with their appearance was 8.4, satisfaction with eating was 8.1, satisfaction with speech was 8.7, and satisfaction with smile function was 7.1. The researchers also report that four patients were physician-graded as excellent to superb.
“Because of the limited number of patients in the study, I think that the procedure will still need to be studied and more patients need to undergo the procedure.” Azizzadeh says. “Furthermore, we will need to also see the long–term results. The surgery will likely be a more challenging operation than the traditional temporalis transfer and static sling, and will likely require a steeper learning curve by the surgeons.
“The indications for the surgery will also be limited to older patients with complete facial paralysis,” Azizzadeh continues. “Younger individuals with complete facial paralysis are much better served with cross facial nerve grafts and gracilis free flaps, which can provide spontaneous facial movement.”