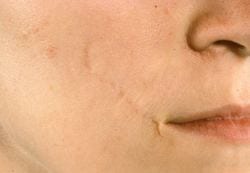
A depressed scar of the right cheek with noticeable contracture on smiling view was treated with a geometric broken line closure followed by dermabrasion.

One year postop. PHOTOS COURTESY OF THOMAS D. WANG, MD
As with everything done in cosmetic and reconstructive surgery, a satisfactory outcome with scar revision begins with a detailed analysis and correct diagnosis of the problem. Only then can you develop a successful treatment strategy.
Scar revision involves much more than simply excising a scar and doing a better closure of the wound. Successful scar revision is really all about disguising the fact that a scar is present and will always be present. It is a matter of tricking the observer’s eye into overlooking or ignoring the scar’s presence.
To get an update on the state-of-the-art in scar revision and scar-revision procedures, PSP spoke with Tom D. Wang, MD, current president of the American Academy of Facial Plastic and Reconstructive Surgery (AAFPRS).
Wang is also a facial plastic and reconstructive surgeon in both private practice and with the Oregon Health and Science University (OHSU) in Portland, as well as a teacher who has been invited to speak both nationally and internationally about cosmetic and reconstructive surgery. In addition, he has been published in medical journals and textbooks.
Wang is certified by the American Board of Facial Plastic and Reconstructive Surgery and the American Board of Otolaryngology, and he earned his medical degree from Northwestern University Medical School in Chicago. He also completed his Otolaryngology/Head and Neck Surgery residency at Northwestern. He followed this up with a fellowship in facial plastic and reconstructive surgery at OHSU.
PSP: What are the recent developments in the use of scar revision or scar removal?
Tom D. Wang, MD: I think there has been greater understanding in aftercare of the wound following surgical intervention. This understanding will allow a more optimized healing, including the use of long-term occlusal modalities—like scar gels or sheets, which can help decrease the redness and the thickening we see in scar tissue.
Relatively recent, within the last 5 years or so, these types of products and treatments have become more popular as far as helping the patients with their scars heal more quickly than usual.
PSP: Are there any sheets, gels, or artificial types of tissues you use?
Wang: Over-the-counter products—scar gels, creams. There are a number of products. They are all pretty similar. They all are basically designed to provide occlusions over the wound, which then traps moisture and makes the immediate scar environment more humid. This seems to decrease inflammation and accelerate scar restoration. I do not have any specific brand preference or any specific manufacturers that I feel do a better job than another. I think they all are very similar.
It’s not really complex technology. It’s pretty simple, but it is something that as physicians we are just beginning to recognize to be more and more useful for our patients.
PSP: Are you using tissue sheets or organic tissue in scar healing?
Wang: Not as much at this point. The new thing is laser technology. It helps to decrease inflammation and redness in fractionated fashion. It seems to be really effective for treating scar-protected inflammation. That is something that is really quite new and something we are excited about.
PSP: Describe how it works.
Wang: In general, the placement of a laser beam helps deal with the blood vessels around the scar area tissue. In that manner it tends to break down the excess in collagen deposition and decrease scar recognition, which is the exact mechanism.
PSP: Does dermabrasion fall under the same category?
Wang: Dermabrasion is a well-utilized procedure modality for scar revision, and it is typically done probably 3 months or so after the surgical intervention for best results. It helps to smooth the surrounding tissue, therefore camouflaging it better. It is an old technique that is very useful and one that I employ routinely.
PSP: What about scars that have matured and are treated years later? What approach can be taken?
Wang: Scars that no longer actively remodel can be treated years later if they are objectionable, or if they are causing ecstatic or friction impairment. Treatment options include that of the traditional scar-revision surgery—excising the scar either on its own or in a pattern, which may help decrease some contraction issues. Then, following up once the surgical part has been done and we have converted the whole mature scar into a fresh one. We returned the hand of the clock back to zero, and it starts ticking from that point forward.
Months later, we could consider dermabrasion if the scar is in the part of the face that is immutable to that. Also, there is the use of scar gels or scar sheets on a long-term basis, usually about 6 months, to help minimize inflammation.
The use of the laser beam treatment in a fractionated pattern is still being established. But the preliminary studies are encouraging.
PSP: Would you say swelling is a major complication after scar removal or scar revision?
Wang: Yes. Certainly, it can be. Edema and swelling can occur after scar revision. We do everything we can to minimize that by the use of the ecstatic agronomic surgical technique, as well as the suture materials to keep edema and swelling to a minimum.
PSP: Looking ahead, where do you see the techniques and technology heading? What would you like to see happen in the more distant future?
Wang: I think it would be wonderful to accelerate the wound-healing process. We have some regenerative enzymes and tissue-growth factors which show promise, but really it’s far too early to have a predictable, reliable clinical application.
For instance, if we were to have a scar that was revised after around the time of the closure, then we could sprinkle in the tissue growth factor, which would allow the wound edges to heal in an accelerated fashion. This will shorten the overall healing time and lead us to the final outcome more quickly.
It would make the recovery time more easy for the patient and, of course, give us the results sooner rather than having to wait 12 months. This would be something on the horizon, and there is promise in that area.
I think that scar revision is a powerful and useful tool to manage unfavorable scar tissue that patients and their providers may not be aware of. After a patient obtains lacerations or injury, he or she may just be happy to have the episode behind them. However, the scar that is left can be a sort of tail sign. By means of diminishing them, it helps the patient physiologically.
PSP: So one of the goals of this procedure is to bring the patient to a better self-image?
Wang: Yes it is, exactly.
Shae Waddell is a contributing writer for PSP.She can be reached at . Jeffrey Frentzen is the editor of PSP. He can be reached at .