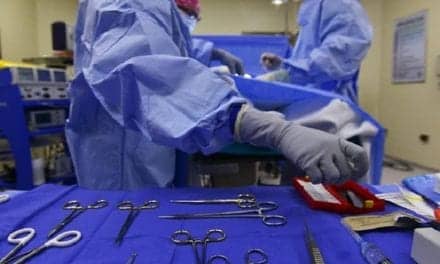
Large-volume abdominal liposuction can be very effective, but it is not a solution for the metabolic abnormalities of obesity

Obesity is assessed using the body-mass index (BMI), which is determined by dividing the patient’s body mass in kilograms by the square of the height in meters. A BMI of 30 or more denotes obesity, and a BMI of 35 or more indicates morbid obesity. Obesity, of course, is a serious health issue that increases the risk of metabolic abnormalities and a wide range of diseases.
LVL creates an opportunity to help many obese patients, but much research still needs to be done. By understanding the general findings of a 2004 study that evaluated the effect of liposuction on insulin levels and risk factors for coronary heart disease,2 clinicians can help set reasonable expectations for patients interested in the procedure.
Reasonable Expectations
Obesity now appears to be an epidemic condition in the United States, so it is important to understand the causes of its prevalence. The reasons for obesity are many. They include abundant, affordable, high-calorie fast food; sedentary jobs; poor levels of participation in exercise and physical activity; and inability to adhere to diet regimens.
Very few people are able to sustain diet- and exercise-induced weight loss over the long term. I have observed that only surgery has achieved consistent, lasting weight loss. Over the past several years, several surgical procedures that restrict food intake or limit food absorption have been developed. These procedures induce dramatic weight loss and rapidly improve obesity-related problems such as type II diabetes, hypertension, and cardiovascular risk factors.
Depending on the type of surgical procedure used, and the patient’s compliance with recommendations for dietary restrictions and exercise, individuals may lose 40% to 70% of their excess weight. Patients who have an initial BMI of 35 to 40 may achieve a BMI of 25 to 35.
Regardless of their final BMI, individuals who lose 32 to 68 kg of weight are left with dramatic excesses of skin, creating aesthetic and functional problems. Patients whose BMIs stabilize at 25 to 32 are typically ideal candidates for excisional surgery to remove troublesome excess skin. Those with BMIs of more than 35 are less-optimal candidates.
To complicate matters, individuals do not lose weight uniformly. Some may lose their excess fat in the trunk, but not in the extremities. Others lose weight, but stabilize at weights too high to make them good candidates for the surgical procedures designed to correct their deformities. However, many of these patients can be helped by liposuction.
Traditional liposuction was designed to remove relatively small excesses of unwanted fat from local accumulations in normal-weight patients. The development of the tumescent technique, in which a large volume of epinephrine-containing fluid is injected to decrease blood loss, has allowed large amounts of fat to be removed safely.
The tumescent technique also lets surgeons convert patients with insufficient weight loss into better candidates for skin-excision procedures. Suction lipectomy to debulk excess residual fat is an additional procedure, and it can significantly improve the results.
Enter LVL

Once weight loss is adequate, as a result of gastric bypass surgery or suction-assisted lipectomy, excisional procedures can produce significant functional and cosmetic improvement. Most weight-loss patients need multiple procedures on several anatomical areas. When the BMI is 25 to 32, several areas can often be corrected during a single operation. When the BMI is more than 32, multiple operations are usually needed.
The core reconstructive procedure for patients who have undergone massive weight loss is the circumferential body lift, which excises the excess abdominal skin and fat and recontours the lower flanks and back. Subsequent procedures usually address the excess skin on the arms, axilla, breasts, and thighs.
Because of metabolic changes and nutritional deficiencies, wound healing and tissue elasticity are abnormal in some bypass patients; some recurrence of skin laxity is the norm. This frequently creates the need for touch-up procedures designed to achieve further improvement.
Despite the need to undergo multiple operations, however, most patients who have undergone gastric-bypass surgery and LVL indicate high levels of satisfaction with the results of these procedures, in my experience.
Certainly, one consideration in any LVL case is postsurgical change in risk factors for disease. Educating patients before procedures usually helps relieve anxiety and promote reasonable expectations. Patients equipped with knowledge make better decisions.
Satisfied patients are typically those who receive pertinent information such as the results of the 2004 study.2 In consideration of this study, a surgeon would tell a candidate for LVL that the procedure does not improve obesity-related metabolic abnormalities but does improve the appearance of the abdominal area.
Study Methods
To measure the effect of abdominal liposuction on metabolic abnormalities, the study evaluated the insulin sensitivity of the liver, skeletal muscle, and adipose tissue (using the euglycemic–hyperinsulinemic clamp procedure and isotope-tracer infusions) prior to surgery in 15 female patients.2 The participants were evaluated again 10 to 12 weeks after surgery. The study subjects were also evaluated before and after surgery for inflammatory risk-factor levels for coronary disease.
The study enrolled patients whose body weights had been stable for at least 2 months and who had been sedentary for at least 6 months. Of the 15 subjects, seven had type II diabetes (BMI: 39.9 ± 5.6) and eight had normal glucose tolerance (BMI: 35.1 ± 2.4); none showed evidence of other serious illness or organic dysfunction. The subjects with diabetes were being treated using a combination of two or three oral medications.
Each patient proceeded with large-volume tumescent liposuction 1 week after the euglycemic–hyperinsulinemic clamp procedure. To induce vasoconstriction—which helps reduce bleeding—the patients received subcutaneous injections of lactated Ringer’s solution that contained 1 ppm epinephrine.
Both superficial and deep subcutaneous abdominal fat were removed—along with small areas of fat in the arms, flanks, hips, or thighs—in five glucose-tolerant patients and four patients with diabetes. The total volumes aspirated ranged from 11 to 13 L from the upper body and from 2 to 6 L from the lower body in glucose-tolerant patients, and from 14 to 18 L from the upper body and from 0 to 2 L from the lower body in patients with diabetes.
Study Findings
The liposuction procedure significantly decreased the subjects’ body fat; it resulted in a 44% decrease in the volume of subcutaneous abdominal adipose tissue for subjects with normal glucose tolerance and a 28% decrease for subjects with diabetes. Further, within 12 weeks of surgery, body-fat mass had decreased 9.1 ± 3.7 kg from baseline in glucose-tolerant patients and 10.5 ± 3.3 kg in patients with diabetes.
Waist circumference was significantly reduced in both groups of patients. Plasma leptin concentrations were also decreased in both groups. The procedure, however, did not affect the concentrations of other circulating cytokines or C-reactive protein.
In contrast, traditional obesity-treatment plans result in decreased plasma concentrations of C-reactive protein, interleukin 6, and tumor-necrosis factor. The concentration of adiponectin also tends to increase as a result of traditional obesity treatment.
Results of this study indicate that leptin production over time is influenced by total fat mass. Liposuction improves the appearance of the treated area, but it is not a substitute for clinical treatment. For example, traditional diet plans that produce weight loss decrease hepatic and muscular fat content, fat-cell size, visceral fat mass, and circulating concentrations of proinflammatory cytokines.
Whether liposuction will produce the metabolic benefits that are often associated with traditional weight loss in women is unclear. Although there is disparity within the 2004 study, it can serve as a foundation for further exploration by surgeons treating obesity. PSP
V. Leroy Young, MD, FACS, is in private practice at the BodyAesthetic Plastic Surgery and Skincare Center and is on staff at Barnes-Jewish West County Hospital, both in St Louis. He is the chair of the ASPS–ASAPS joint task force on emerging trends and of the ASAPS committee on nonsurgical procedures. He can be reached via his Web site, www. bodyaesthetic.com.
References
1. Anne Collins Weight Loss Program 2006. Obesity statistics. Available at: http://[removed]www.annecollins.com/obesity/statistics[/removed]-obesity.htm Accessed March 17, 2006.
2. Klein S, Fontana L, Young VL. Absence of an effect of liposuction on insulin action and risk factors for coronary heart disease. N Engl J Med. 2004;350:2549–2557.