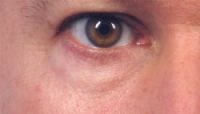
Figure 1. One cc of hyaluronic acid filler (Perlane) was injected deeply along the tear trough and infraorbital rim.
Contrary to the labeling found on many over-the-counter eyelid creams, there is no cure-all for lower-eyelid dark circles. The patient who complains of a tired appearance related to the lower lids often presents with a constellation of findings. These may include thin skin, pigmentary collections, subcutaneous fat atrophy, visible eyelid vasculature, prominent orbital fat pads, deep-set globes, dynamic orbicularis muscle bulges, orbital rim definition, and light/shadow interplay.
It would take one incredible cream to target all of these issues.
PRESERVING THE PAST
Fortunately, not every eyelid crease and shadow needs to be targeted with a treatment. An orbicularis roll, for example, is often a youthful sign and should be preserved in many cases. The same goes for a lower-eyelid crease, which is common in children and can persist in adulthood.
In a consultation, patient photographs taken 10 years earlier (rather than 30 years earlier) may reveal some of these youthful elements, and are valuable when assessing the anatomic progression and setting a realistic end point.
Other contours seen in youthful faces can be accentuated with advancing age, as with the so-called tear trough. This depression, also termed the nasojugal fold or groove, sweeps in an inferolateral direction from the medial canthus, as it overlies the inferomedial rim of the bony orbit.
Aging can emphasize the normal contours of this area, leading to unfavorable shadowing. This is particularly the case in patients with malar hypoplasia, a negative vector relationship, subcutaneous fat atrophy, and/or protruding orbital fat. When considered in conjunction with the surrounding aesthetic subunits (including the lower-eyelid and cheek components), the tear trough can be the target of procedures that are both natural and rejuvenative.

Figure 2A. A subperiosteal pocket is initiated over the orbital rim from a transconjunctival approach.

Figure 2B. A medial orbital fat pedicle is created for redraping.
FILLING IT UP
Injectable hyaluronic acid fillers have grown in popularity and can effectively soften the appearance of the tear trough (Figure 1). Most physicians advocate the practice of deep injections in this area to avoid filler visibility or a Tyndall effect. In the depth of the trough, orbicularis muscle is firmly adherent to the periosteum of the orbital rim. Overinjection in the tight preperiosteal plane, particularly in bolus form, can lead to intraorbicularis mounds, which may be smoothed with manual pressure. In select cases, injections performed in the supraorbicularis plane can be helpful and should be deposited in small threads or aliquots because lumps are easily seen through the thin eyelid skin.
The durability of this procedure is impressive, and I have seen the volumizing effect of hyaluronic acid fillers in the tear trough for longer than a year after a single treatment. I keep hyaluronidase available in case of irregularities or discolorations, but I have rarely used it.
REDRAPING


Figure 3. An infraciliary approach was used to redrape orbital fat followed by fat transfer by injection and fractional laser resurfacing.
In patients with moderate to severe medial fat pad protrusion and deep tear troughs, the injectable approach may be inadequate. If excellent skin and orbicularis tone are present, I favor the transconjunctival route to surgical fat rearrangement as described by Goldberg in 2000. A subperiosteal pocket is initiated at the inferomedial orbital rim and extended to the anterior aspect of the maxilla beyond the tear trough (Figure 2A). Orbital fat pedicles are mobilized and repositioned (Figure 2B) using securing sutures, as needed. I use 5-0 polyglactin sutures for internal fixation or 5-0 polypropylene sutures externalized over a bolster. A nice balance is often achieved by reducing the fatty “hills” and elevating the deep “valleys” at the same time.
If the skin and orbicularis muscle exhibit more advanced involutional changes, I opt for the transcutaneous approach to orbital fat redraping. This allows me to address orbicularis laxity and lower-eyelid skin redundancy. Many surgeons are reluctant to create a lower-eyelid scar, but I find that a well-placed infraciliary or lower-eyelid crease incision is barely perceptible (Figure 3).

Figure 4. Fractional CO2 laser resurfacing after transconjunctival fat redraping.
Eyelid malposition after “anterior” blepharoplasty is a well-known concern. As a rule, I add support to the lower eyelid with canthal tightening and/or orbitomalar suspension during an anterior-approach blepharoplasty.
When there is not enough orbital fat, repositioning alone may not result in an optimal contour at the lid-cheek transition zone. Autologous fat transfer techniques will aid in blending the adjacent areas. I often graft harvested fat to the cheeks, brows, and temples at the same time as lower blepharoplasty. If bulging orbital fat pads are absent (frequently seen after prior reductive blepharoplasty), fat may be transferred directly to the tear trough in the suborbicularis and intraorbicularis planes.
LASER PRECISION
Fractional carbon dioxide laser resurfacing has become a cornerstone of my lower blepharoplasty technique (Figure 4). A combination of deep and superficial ablation modes are used to improve dyschromias, fine and deep rhytids, and textural issues related to actinic damage. These surface improvements act to further reduce tear trough visibility. I have not seen any difference in downtime when fractional laser treatment is added to blepharoplasty—and a synergistic effect often ensues.
In situations where lower eyelid dark circles are caused by multiple factors (which is almost always the case), a combination approach that addresses the specific findings seems to work best.
If there was a single “magic” cream for dark circles, everyone would know about it and it wouldn’t be hidden in the back of magazines or sold exclusively via spam e-mails. For now, the next best thing to an expertly performed cosmetic eyelid procedure is a topical concealer.
Brett Kotlus, MD, MS, is a cosmetic and oculofacial plastic surgeon who is board-certified by both the American Board of Cosmetic Surgery and the American Board of Ophthalmology. He practices in Shelby Township, Mich, and can be reached at (586) 992-8300 or www.eyeliftcenter.com.
FURTHER READING
- Facial recontouring with autogenous fat. Facial Plast Surg. 2004;20(2):145-147.
- Tranconjunctival orbital fat repositioning: transposition of orbital fat pedicles into a subperiosteal pocket. Plast Reconstr Surg. 2000;105(2):743-748.
- The tear trough and lid/cheek junction: anatomy and implications for surgical correction. Plast Reconstr Surg. 2009;123(4):1332-1340.
- Dual-depth fractional carbon dioxide laser resurfacing for periocular rhytidosis. Dermatol Surg. 2010;36(5):623-628.