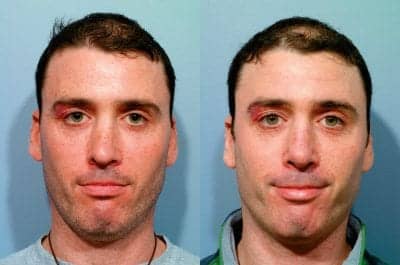
This 36-year-old patient had two prior nasal operations with a nasal fracture between, with a very deviated septum, crooked asymmetric nasal tip, crooked middle vault, inverted V deformity, open roof bony deformity, and saddle nose. Reconstructed with grafts from his rib. Photos courtesy of Steven J. Pearlman, MD, FACS
What are the most common reasons that lead patients to seek revision rhinoplasty?
A long list of complications in rhinoplasty has been identified over the years by revision rhinoplasty specialists in lectures and publications. However, these complications have mostly been identified as singular topics in medical texts and journals, or identified when being presented through discussion of an advanced surgical technique.
Revision rhinoplasty is a unique and specialized discipline within facial plastic and reconstructive surgery, correcting untoward results of what is often considered the most difficult procedure in cosmetic surgery.
The importance of this issue is underscored by the reported incidence of revision rhinoplasty in the medical literature ranging from 5% to 15%.1-4 What makes this an even more ominous number is that the authors publishing these articles are usually surgeons who perform the most rhinoplasties in the first place, which likely means that the incidence is even higher for the occasional rhinoplasty surgeon.
For both primary and revision surgery of the nose, the surgeon must address not only aesthetic issues but function in every case, even if not evident. All too often, patients are offered “simple” or cookbook solutions to primary and secondary nasal defects that may end up making the situation worse—as well as making further revision more complex. Even a slight narrowing of the nasal sidewalls can sometimes reduce airflow to normal airways. Surgeons who perform both primary and revision rhinoplasty must understand the consequences of all surgical maneuvers performed on the nose. There are also heightened emotional concerns of patients who report that they have been “traumatized” by one or more previously undesirable results.
The medical literature is replete with studies that identify and evaluate objective “deformities” from the perspective of the surgeon, and subsequently discuss revision techniques specific to the recognized deformity. These articles delineate the most common aesthetic abnormalities in multiple-revised noses.



AESTHETIC CONCERNS
The most commonly reported aesthetic abnormalities are poly-beak deformity, depressed tip, tip contour irregularities, bossae, over-rotated or under-rotated nasal tip, dorsal irregularity, residual hump, retracted ala or columella, hanging columella, wide base, and implant displacement.1,2,5,6
The most common stigmata of an “overoperated” nose recognized by presenting patients are listed in the table on page 19. When patients present, they often report a number of these findings. Although these analyses are important, they are all retrospective and subjective in nature, and report from the surgeon’s point of view. Thus, these studies may not reflect the patient’s primary reasons for pursuing revision rhinoplasty.
Kathy Yu, MD, Alyn Kim, MD, and I authored a study on this issue, “Functional and Aesthetic Concerns of Patients Seeking Revision Rhinoplasty,”7 which appeared in the September-October 2010 issue of the journal Archives of Facial Plastic and Reconstructive Surgery. Patients seeking revision rhinoplasty have a number of concerns. The foremost are poor aesthetic and functional results. Second comes from loss of trust in their first surgeon; the third is that further surgery may cause further deformity. Regarding the third issue, patients will often bring up the late pop artist Michael Jackson—illustrating a fear that almost every patient, or a relative or friend of theirs, will eventually bring up when considering revision rhinoplasty.
Our study asked 104 consecutive patients presenting for revision rhinoplasty what they are unhappy with. We sought to address patients’ concerns directly rather than what authors and surgeons feel might be the surgical priorities. Patients seeking revision rhinoplasty were given a questionnaire prior to consultation with me at the time of their first visit. This included more than 40 potential problems, so that the evaluation would not influence the patients’ answers.
Patients were then examined. Validated survey results were compared with the surgeon’s findings in a chart review. In addition to choosing all presenting concerns, patients were asked to rank the top three concerns motivating their desire for revision surgery.
Two separate charts were compiled. First were all patient concerns. The second reflected what patients considered most important to them. The most common aesthetic findings in order of frequency were the following:
- Tip asymmetry;
- Crooked middle third of the nose; and,
- Upper-third irregularity.
When adding functional complaints, 64% of patients presented with nasal obstruction. An even greater amount—71% of the total patient population—had nasal obstruction on evaluation. When asked to narrow it down to the three most bothersome concerns, patients selected nasal tip asymmetry, nasal obstruction, and a crooked middle third of the nose (in that order of importance).
In our study, all aspects of the nose played a role in why patients sought out revision surgery. First and foremost was the nasal tip. A crooked nasal tip may result from initial asymmetry of the tip cartilages, underlying dorsal septal angulation, or asymmetrical scarring of the skin-soft tissue envelope. Persistently wide nasal tips may be just that or related to poor nasal tip definition, as reported by patients representing perceptions regarding tip scar tissue, bossae (knuckles at the end of the tip), alar retraction, and/or deepened alar creases.
Middle third nasal abnormalities were the most common cause of functional complaints from nasal valve problems as well as a crooked middle third or narrowed middle third, creating an “inverted-V” deformity. These problems may arise from deviation of both the central part of the nasal septum that affects airflow, the dorsal aspect of the septal L-strut and its role in lower 2/3 angulation, and position and strength of the upper lateral cartilages.
Upper or bony nasal irregularity stems from the unforgiving nature of the nasal bony pyramid. Treating the nasal bony pyramid is not like sanding wood. Bony reactions during healing may restore portions of the nasal hump. Osteotomies for upper-third angulation may recur from persistent crookedness of the central nasal structures, or sometimes fail to close an open roof deformity. Even slight angulation of an osteotome can cause excess hump removal.





A 46-year-old patient with one prior septorhinoplasty. Notes: Deviated septum; wide nasal tip with bossae (5 mm of cartilage was present and “scored,” according to the op note); and alar narrowing. The middle third is slightly crooked; the dorsum is normal.
FUNCTIONAL COMPLAINTS
In addition to aesthetic concerns, the most common functional problems encountered in revision patients are a deviated septum, nasal valve collapse, nasal septal perforation, and synechea. Each of these findings must be looked for and treated if present. It surprises me that when examining patients, I ask if their original surgeon ever looked inside their nose, and the answer is, sometimes, “No, my surgery was only aesthetic, so the surgeon didn’t have to.” All too often, a deviated septum is present and the patient didn’t realize its functional deficits; or, it may become a problem with even a slight narrowing of the nasal sidewalls.
Sometimes even minor narrowing can make a difference in nasal function. The nasal airway functions according to the Poiseulle’s equation (DP=n8L/pr4): Pressure along a tube (nasal airway) is inversely affected by the radius to the fourth power. As the nasal airway sidewalls and subsequent airway are reduced by surgery, a previously asymptomatic deviated septum or even slight narrowing of the nasal valve may have a significant effect on airway pressure and subsequent collapse when the Bernoulli Effect of airflow pulling inward on the sidewalls of a cylinder is applied.
At the end of our survey, we asked patients why they didn’t go back to their original surgeon. The most common answer was because the first or most recent surgery was not successful. The second most common reason was the original surgeon was not receptive to their concerns.
Revision surgeons and their staff need to be more sensitive to patients who are unhappy with their results and the other surgeon’s results. Often, patients wait many years before even considering revision surgery.
There is a common cliché, often attributed to Albert Einstein, in which one definition of insanity is to repeat the same behavior over and over and expect a different result. Patients need to be reassured that although more complex, revision surgery can be rewarding and improved nasal form and function can be restored.
KEEPING IT STRAIGHT
To categorize the most common findings in patients seeking revision rhinoplasty, one must discuss likely causes and briefly present techniques for optimal treatment, including ways to prevent them from occurring in the first place.
As we were taught in our residency, the best treatment of a problem is to avoid it in the first place. The most common presenting problems in revision rhinoplasty go from bottom to top—the lower third or nasal tip, middle nasal vault, and upper bony third of the nose.
By exploring the reasons for revision rhinoplasty, it makes it easier to practice and teach one of the most basic tenets in medicine: Prevention is the best treatment. If surgeons can anticipate potential problems, hopefully most of these problems can be avoided in the first place.
NASAL TIP
Nasal tip deformities seen in revision rhinoplasty stem from vagaries of volume, strength, and shape of the lower lateral cartilages.
Persistence of a wide or bulbous tip is most commonly from too conservative a resection of the lateral crura. At times, deepened alar creases from cephalically oriented lateral crura can also give the appearance of a wide or ptotic nasal tip when the alar cartilages are actually the proper size. When the lateral crura lie at an angle greater than 45° from a horizontal plane, the alae appear separate from the tip and have almost a “stuck-on” appearance.
Patients perceive this by describing a wide tip when it really is of normal width and alae that appear to flare, but really do not. Deep alar creases and cephalic lateral crura can also make the tip appear to plunge downward when the nasolabial angle is measured to be normal. A wide tip can be treated like a primary tip-plasty.
Too narrow a tip, a pinched tip, and bossae result from over-resection of the lateral crura. Unless patients have very strong cartilages, at least 7 mm of lateral crura should remain. Other causes for too narrow a tip can be concave-shaped lateral crura or overtightening of dome sutures. When the lateral aspect of the lateral crura turn inward, cinching the domes tighter with sutures will result in lateral pinching and may also lead to external nasal valve compromise. Primary alar batten grafts may be necessary to prevent this complication.
For an overly narrow or pinched nasal tip, treatment options are alar batten grafts, alar strut grafts, relocating the lateral crura more caudally, and rim grafts.
Asymmetry of the nasal tip occurs from three primary causes. The first is underlying angulation of the end of the nasal septum. (To quote my mentors, William Lawson, MD, and William Friedman, MD, “As the septum goes, so goes the nose.”) The second cause is misplacement of dome sutures; and the last and least common is pre-existing asymmetry of the lower lateral cartilages.

Nasal tip projection can be excessive or inadequate. Most maneuvers performed on the nasal tip and adjacent structures have some effect on nasal tip projection. To impart minor reduction in projection, the following can be used: skeletonization of the nose, cephalic resection of the lower lateral cartilages, and severing tip-supporting ligaments.
Other techniques that have greater effects in reducing tip projection include incising the lateral crura, significant shortening of the nasal septum, dome truncation, and nasal spine removal. To predictably increase projection, cartilage grafts are usually necessary. The best way to prevent inadequately addressing tip projection is to have a full understanding of the Anderson Tripod theory of nasal tip support.8




This 24-year-old patient with two prior rhinoplasties demonstrating 5/7 stigmata. Her concerns: Nasal tip poorly defined with “bumps” (and “hard and pointy”), and asymmetric middle third and visible nasal bones. My findings: Wide nasal bones, crooked middle third with inverted V deformity, crooked, overprojected nasal tip with bossae and alar narrowing, deep alar creases, and “shrink-wrapping” of nasal skin.
Nasal tip rotation refers to the nasolabial angle and maintaining, raising, or lowering the nasal tip. Over-rotation of the nasal tip typically occurs when the lateral crura are either transected or reduced excessively so that they buckle. Minimal tip rotation is achieved by the following: cephalic trim of the lower lateral cartilages, caudal resection of the upper lateral cartilages, hump removal, and dome sutures.
More significant tip rotation requires interruption of the lateral crura and can also be accomplished by the use of a columellar strut and extended shield grafts. Over-resection of the caudal nasal septum also contributes to excess rotation. The tongue-in-groove technique can also significantly affect tip rotation and projection. Prevention of over or under tip rotation is best accomplished by a full understanding of nasal tip support, as indicated above, and the mechanisms by which nasal tip rotation occurs.
MIDDLE NASAL VAULT
Middle nasal vault problems arise from underlying angulation of the nasal septum, internal nasal valve compromise, or an imbalance of nasal structures on profile. Sometimes, the nose appeared straight before surgery and is no longer straight afterward. This is due to deviation of the nasal septum going all the way up to the dorsum of the septum or the top.
We usually address only the middle and lower portions of the septal cartilage and bone when correcting a deviated septum. However, when the pyramid of the nasal bones and upper lateral cartilages are lowered, as in a hump removal, these side structures reattach to a lower part of the septum. If this is crooked, it ends up shifting the midline off-center. A once straight nose now becomes crooked.
A careful intranasal exam with a speculum and illumination or even nasal endoscopy can diagnose this potential problem at the time of the initial examination. Spreader and/or onlay grafts can help treat or camouflage this condition.
A narrow internal nasal valve has both functional and aesthetic consequences. Aesthetically, this manifests as an inverted “V” deformity. Possible causes are displacement of the upper lateral cartilages, large hump removal, and excess narrowing of the bony dorsum.
Predisposing conditions that can lead to middle vault problems are short nasal bones and tension nose deformity. A tension nose has a high, narrow middle vault that may have visible inward motion on forced breathing. Prevention and treatment is a controversial issue. I feel that pre-emptive use of spreader grafts helps reduce the occurrence of these complications.
Poly-beak deformity results from lack of support or balance of the nasal structures when viewed on profile. The dorsal septal cartilage may be too high; the nasal bones may be too low (bony abnormalities), or unanticipated loss of tip support (tip projection). Thick skin may also heal with excess scar tissue in the supratip areas.
The first two circumstances are addressed elsewhere. The skin over the rhinion is thinner than in the supratip. Dorsal septal resection should incline slightly upward. Slightly more cartilage should be removed caudally to obtain a straight profile.
For patients with thick skin, compensation should be made by excising more cartilage to allow room for healing and more scar tissue. Careful taping and postoperative use of steroid injections will also help.
BONY NASAL VAULT






The upper third of the nose is the bony nasal vault. Frequent deformities encountered in this area include open roof, persistent angulation, saddle nose, irregularity, and persistence or recurrence of dorsal hump.
When more than a slight hump is removed, lateral osteotomies are necessary to close the roof. Patients often ask if we have to “break the bones.” To obtain a good result, this is necessary in most cases when there is hump removal. A simple explanation of the necessity of this maneuver in obtaining a superior result should suffice. Irregularities can be reduced by the use of sharp rasps and osteotomes.
Upper third angulation results from high central bony septal deviation. A cross-nasal osteotomy will treat this situation. Saddle nose deformity (or over-resection) occurs when too much bone has been removed. I feel that this results from aggressive use of an osteotome. If the surgeon’s wrist is held too high, too much bone will be removed. Try removing less bone and follow up with a rasp, or use only rasps until the precise angle for an osteotome can be assured.
The last condition I will address is persistence of a small bony hump after rhinoplasty. The bony-cartilaginous junction or keystone area is a complex region of the nose and must be carefully examined after hump removal.
Regrowth of a hump after rhinoplasty is often blamed on incomplete resorption of the bony callus. This may be an excuse, but dorsal humps seen after nasal trauma without visible fracture gives evidence that this truly occurs. Unfortunately, I do not know how to prevent or recognize when this situation is going to arise, which makes prevention difficult.
CONCLUSION
When it comes to rhinoplasty—both primary and revision—the first thing is to assure or restore strength and structure. This is in contradistinction to what was done back in the 1970s and 1980s, during which the motto was “remove, remove, remove.”
Much of what we now know comes from looking back and seeing what happened when too much was removed. Noses were reduced to the smallest or lowest point for a balanced shape. All too often, these techniques are now recognized to compromise both function and aesthetics.
Primary and revision rhinoplasty follow the theme of Modernist architecture, or “form follows function.” Noses that look pinched typically don’t work well, and vice versa. Improving nasal airflow has the consequence of also enhancing the appearance of the nose. Each maneuver used during rhinoplasty should have a purpose, since each has multiple consequences. For example, altering the lateral crura can affect nasal tip width, projection, and rotation.
Other considerations, not addressed in this article but also important, especially include nasal obstruction, nasal length discrepancies, and columellar and alar deformities. My hope is that some of the above-mentioned tips and techniques will help you reduce the incidence of untoward results in rhinoplasty.
Steven J. Pearlman, MD, FACS, is dual board certified in both facial plastic and reconstructive surgery and in head and neck surgery. A former president of the American Academy of Facial Plastic and Reconstructive Surgery, he is in private practice in New York City, and can be reached at (212) 223-8300 or www.mdface.com.
REFERENCES
- Thomson C, Mendelsohn M. Reducing the incidence of revision rhinoplasty. J Otolaryngol. 2007;36(2):130-134.
- Kamer FM, McQuown SA. Revision rhinoplasty: analysis and treatment. Arch Otolaryngol Head Neck Surg. 1988;114(3):257-266.
- Bagal AA, Adamson PA. Revision rhinoplasty. Facial Plast Surg. 2002;18(4):233-244.
- Vuyk HD, Watts SJ, Vindayak B. Revision rhinoplasty: review of deformities, aetiology and treatment strategies. Clin Otolaryngol Allied Sci. 2000;25(6):476-481.
- Foda HM. Rhinoplasty for the multiply revised nose. Am J Otolaryngol. 2005;26(1):28-34.
- Constantian MB. Differing characteristics in 100 consecutive secondary rhinoplasty patients following closed versus open surgical approaches. Plast Reconstr Surg. 2002;109(6):2097-2111.
- Yu K, Kim A, Pearlman SJ. Functional and aesthetic concerns of patients seeking revision rhinoplasty. Arch Facial Plastic Surg. 2010;12(5):291-297.
- Anderson JR. The dynamics of rhinoplasty. In: Bustamant GA, ed. Proceedings of the Ninth International Congress of Otorhinolaryngology, Mexico City, August 10-14, 1969. Amsterdam, the Netherlands: Excerpta Medica; 1970.
ADDITIONAL TABLES
Nasal Tip Deformities

Middle Nasal Vault Deformities

Upper Third, Bony Deformities