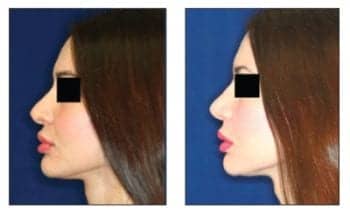
Figure 1. To correct relatively minor imperfections, the anterior cartilagenous dorsum was shaved down, followed by resecting the anterior-inferior septum, which was depressing the columella.
Between 20% and 25% of all rhinoplasty patients are unhappy, according to recent data compiled by the American Academy of Facial Plastic and Reconstructive Surgery (AAFPRS). That is not good advertising for cosmetic surgery. Such a failure rate is unacceptable in other surgical specialties. We need to ask ourselves why we, as a group, are not performing better. My sense is that we need to review the history of the procedure, its evolution, and then draw some conclusions that hopefully can help us improve our batting average.
Currently, we are seeing widespread rhinoplasty performed by the third generation of surgeons. The first generation, practicing in the 1950s and 1960s, working on the core precepts and technique of Jacques Joseph, a refugee from Germany, brought rhinoplasty to the public as a procedure within economic reach of the middle to upper-middle class. In those early days, total fees were less than $1,000.
This generation included Parkes, Fuchs, and Holden in Los Angeles; Tresley, Ariagno, and Tardy in Chicago; Diamond, Safian, and Rees in New York City; among others. They opened the doors to the rhinoplasty operating suites during the expansive, post-World War II American heyday.
The second generation of surgeons took the procedure to another quality level and expanded its popularity by refining the techniques and developing variations upon Joseph’s core precepts. This generation’s noses were less overdone and looked more natural, and thus this procedure’s appeal ever broadened.
The use of cartilage, fascia, and bone grafts now allowed surgeons to better deal with primary or secondary deformities. Man-made implants to augment the dorsum, columella, and tip were welcomed deliveries from the biotech world. The open rhinoplasty technique, allowing greater visualization of the anterior portion of the nose, allowed better access for insertion of the transplanted tissue as well as the alloplastic implants. For trainees, this approach lowered the complexity threshold.
Today’s surgeons, the third generation, benefit additionally from the availability of the newer “filler” materials that are also doing well in their attack against aging/shrinkage of the facial soft tissues. With better outpatient anesthesia techniques nearly eliminating postop nausea and vomiting, there is even less patient resistance to having the procedure. It’s a good time to be a rhinoplasty surgeon. The toolbox is loaded. The public has now long accepted rhinoplasty as safe, practical, and affordable.

Figure 2. Multiple nasal fractures and two prior reconstructions. Major revision septoplasty, rhinoplasty. Then,months later, sequential filling injections to left alar divot.
WHAT’S THE BEEF?
Despite all these advances, a problem has developed for the cosmetic surgery specialties: a high rate of aesthetically and functionally poor results. So, despite a full plate of handy instruments, imaginative implants, facility in utilizing local, distant solid tissue for reconstruction, and safe and practical liquid fillers, the high rate of justifiably dissatisfied patients is a black mark for cosmetic surgery.
What is wrong here? Why should this be? With its popularity on the rise and with 60 years of universal experience, it doesn’t make sense.
If the tools and products are so good, we need to look at the practitioners. My sense is that the residency training and experience, for some trainees, is substandard and inadequate. Some programs do not offer enough rhinoplasty and related internal nasal surgery experience under well-qualified supervision.
We hear of specialists, new in practice, who happily accept patients for rhinoplasty yet have had fewer than 10 cases’ experience in training. That number is not adequate considering that rhinoplasty is the most technically challenging of all the common cosmetic procedures. It also requires a well-honed aesthetic sense that comes only with superior training and long, focused experience. Maybe not every head and neck or plastic surgeon should be doing rhinoplasty? No more than every plastic surgeon should be doing cleft lip and palate work, nor should every head and neck surgeon be doing stapedectomies. Each field is very broad. Is there too wide a range of procedures to master?
Perhaps the core of the problem is that today’s generation of young practitioners are getting their resident experience, including that of medical education, in a vastly different medical world. Teaching hospitals, which are stressed economically, no longer have the large volume of “teaching patients”—those who traded an operation by a trainee, under faculty supervision, for a rock bottom fee, if any. That limits resident experience. Further, a generation ago many plastic surgeons and head and neck surgeons honed their skills, following residency, in the military. Today, without compulsory military service, few young surgeons gain that enormous advantage.
Most importantly, the reality may be that residency training alone cannot produce the highly skilled rhinoplasty surgeon that the public desires and expects, and of which the profession should be proud. Additional focused training—the fellowship—may be necessary. I suspect that most of today’s most talented and productive rhinoplasty surgeons are fellowship trained. The “finishing school” turns out to be critical.

Figure 3. The classic overdone male rhinoplasty. Diffuse scarring made the prospect of surgery quite daunting. Correction by sequential filling injections only.
CAUSES AND CURES
There are three technical reasons for the failures.
First, too much was done. The early generation of noses were technical achievements but often aesthetic failures. We still see some contemporary noses that wear an invisible sign that reads, “I had a rhinoplasty.”
The dorsum is taken down too low, and the tip is pinched. The tip has been rotated up too much, and the nose may be overnarrowed to almost a pencil-like thinness. Certain personalities in the media have been the poster boys and girls for overdone rhinoplasties in what should be the age of rhinoplasty enlightenment.
In second place are crookedness, irregularities, and asymmetries. Postoperative crookedness, whether pre-existent or a by-product of the procedure, is almost always due to unrecognized or inadequately corrected deviation of the septum. The old saying is still true: “As the septum goes, so goes the nose.” If you are not adept at performing septoplasty to straighten the nose and at the same time improve breathing, you will have a higher rate of poor results and dissatisfied patients. The irregularities and asymmetries come from either unrecognized asymmetries or as the manifestation of the uncorrected deviated septum.
Also, inadequate attention to detail during the operation, whereby unequal amounts of tissue were removed bilaterally and end-of-surgery evaluation did not recognize such. Imperfections can also come from the unpredictable nature of grafted tissue as it nests within the nose. You must have a keen eye for symmetry and use both your tactile and visual senses throughout the operation—particularly at the end. A few minutes’ extra time spent at the operation’s conclusion is always less than an hour or more spent on a revision procedure.
Third, the surgery itself, particularly if a complication of the rhinoplasty is internal nasal valve stenosis, can cause breathing problems. You must also be able to evaluate an airway prior to surgery. You need to recognize the presence of a deviated septum and even also recognize that the turbinates may play a role in nasal obstruction. Often, the septal surgery could be satisfactory and, yet, the patient becomes quite obsessed with a breathing deficiency because other causes of airway obstruction were not managed at surgery.
PATIENCE IN PATIENTS

Figure 4. Third nasal surgery procedure. Besides the refinement rhinoplasty, persistent internal nasal obstruction was corrected by revision septoplasty and limited turbinate resection. Recurrent headaches and sinusitis were cured.
Another reason patients are temporarily unhappy is that often they are impatient and expect that the final result of rhinoplasty will appear—almost magically—immediately after surgery. Some cases require many months of ripening and maturing before the nose achieves its final appearance. Those patients who had a complicated operation or have particularly thick skin will take more time.
You must be neither anxious and impetuous, nor irritated by the patient’s anxiety. Instead, you must reassure your patient that time is in their favor and that, “Good noses, like good wine, take time before they are fine.”
Often, physician and patient patience is rewarded with a satisfactory result without any intervention. Surgical intervention postoperatively should be very rare unless you are facing a serious problem such as a hematoma, infection, or gross movement of implant or grafted material.
You must be confident in your predictions, lest your patient lose confidence. In-office treatments, such as subcutaneous repository steroid injections or fillers, should be called upon, but only after the tissues have softened and can accept these injections. Typically, after the requisite postoperative “100 days,” the tissues are ready to accept injections.
Poor planning and faulty decision-making also contribute to an unsatisfactory rhinoplasty. In reviewing primary rhinoplasty operative reports and studying the sequence of operative steps, it could be determined that you may have failed to anticipate how modification of one portion of the nose will have a bearing on the appearance of an adjacent portion of the nose. A classical example is failure to recognize that tips tend to drop in the postoperative period. If you do not anticipate such and correspondingly lower the cartilaginous dorsum after the desired tip position is set, there is a good change there will be tip ptosis or a pollybeak deformity. You need to decide whether additional support or grafting material may be necessary. But, another variable is now introduced into the equation that yields the end result.

Figure 5. Rhinoplasty followed by a failed attempt at elevation of the left nasal bone. Then, injections of hyaluronic acid shortly thereafter. Improvement by hyaluronidase dissolution of the filler, a several-month wait, and sequential filling injections.
Another indirect cause of dissatisfaction is that inexperienced rhinoplasty surgeons often undervalue operative speed and efficiency. Speed for speed’s sake is not the issue. Rather, if you take too long to execute whatever maneuvers you choose to execute, a negative factor now influences the outcome. The 3- to 5-hour rhinoplasty, with the attendant increased swelling and bleeding and distortion of landmarks, is much less likely to be satisfactory. How can you make good decisions, based on visual criteria, when the tissues are swollen and bleeding? If you are a long-operating-time rhinoplasty surgeon, and ideally always self-critical, you need to examine your particular technique and ask what factors are lengthening the operating time. Often, it is failure to have an outline or game plan in place before the first incision is made.
If you announce, “When I get in there, I’ll figure out what to do,” your OR staff likely knows to order-in lunch because it’s going to be a long case. Architects build or change structures with a clearly written blueprint. You need one, too.
IT’S ALL IN THE APPROACH
Does every rhinoplasty operation need “everything” done? Perhaps we have overvalued the role of tissue grafting and assume it must be routinely executed. While tissue grafts are often essential, not every operation has to have a tissue graft. Not every rhinoplasty has to be performed via the open technique.
There has been a trend toward performing all rhinoplasties using an external, transcolumellar incision. Every incision introduces yet another focus of unpredictability and possible complication. Hence, the more incisions, the more uncertainty of the result since opposing or parallel contractile forces cannot always be accurately measured.
Many rhinoplasties that should be very simple and easily executed become unduly complex because you automatically place a cartilage graft on the tip or spreader grafts on the dorsum, or routinely place onlay grafts onto the bony and cartilaginous dorsum. It is instructive to study Joseph’s classic rhinoplasty technique and then the sentinel article by Diamond. Hump removal, narrowing of the upper lateral cartilages, refinement of the tip cartilages, with possible shortening of the caudal septum, and then osteotomies to narrow the nose are the core processes of a majority of rhinoplasties.
Sometimes, history takes us on strange courses. Mimicking fashion, there are operative trends and fads. Often, then, operations are made more complex than they should. We see this in other cosmetic plastic surgery where once upon a time the platysma muscle was completely transected in face and neck lifting, and all patients were having tightening of the SMAS. These are not always necessary. As a matter of fact, that complete horizontal transection of the platysma, developing the so-called platysma flaps, created an iatrogenic deformity and a host of unhappy patients. Don’t try to fool Mother Nature too much. Being conservative and limiting the number of components to an operation make good sense with respect to predictability and the avoidance of complications.
CONCLUSION
Always consider the great basic principles of surgery. An adequate local anesthetic-vasoconstrictor block, efficiency of execution, atraumatic technique, and following a well-defined game plan with a minimal number of incisions and maneuvers will lead to a more predictable result—and, of course, fewer revision rhinoplasties.
Robert Kotler, MD, FACS, is a board-certified facial plastic surgeon in private practice in Beverly Hills, Calif. He can be reached at www.robertkotlermd.com.