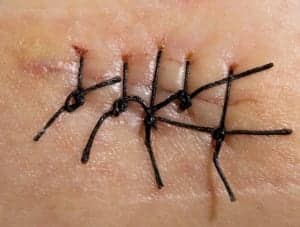
Scar revision can be one of the most complex aesthetic procedures. Depending upon the severity and location of the scar, an extensive combination of techniques may be employed.
Once the skin layers heal, the scar is permanent. However, depending on the location and type of scar, as well as the patient’s skin pigmentation and the age of the scar, scar revision may be an option to remove or reduce the appearance of a scar. It can also restore function and/or correct disfigurement.
Some variations on scar revision include laser therapy, Z-plasty, skin grafting, and dermabrasion. All of these options involve risks to the patient, as well as the possible recurrence or worsening of the scar.
TIMING AND SURGERY
“When looking at a scar, the first question you have to ask is, to whom is it unsatisfactory?” asks Jane Petro, a cosmetic surgeon based in Boston. “Patients always hate scars when they bring them to your attention. But in fact, the scar may represent the best healing possible. So, history of the injury, course, and duration of the healing process must be analyzed if repeating unsuccessful outcomes are to be avoided,” she explains.
“At 6 weeks after any incision in the skin, all scars will look unsatisfactory, and that appearance may continue for several months,” Petro continues. “Thereafter, the question is, ‘What about if the scar is unsatisfactory?’ “A simple line, with redness and some thickness, may just be slight hypertrophy, and time, massage, silicone sheeting, or triamcinolone injections will all result in improvement. A thicker line, with more redness, itching, pain, and tenderness may be an early keloid, helped again with the above but requiring careful monitoring.
“With these scars, before surgical revision is decided, it is important to determine why it remains red and raised. Was there a reaction to the suture material? Is the patient a picker? Is it in an area of the body notorious for such scars—anterior chest, shoulder areas, earlobes? Was there delayed healing the first time, or wound infection?
“Positive answers in these areas should result in a surgical plan designed to avoid repeating those issues. Careful surgery, good approximation, use of monofilament suture with low reactivity—avoid Vicryl and Chromic sutures—avoidance of tension, and close follow-up for several months are essential.”


Figure 1. Gored by a deer antler, this patient was treated with a single treatment of three passes of multipass, high-fluence, high-density CO2 laser resurfacing. This extent of improvement is rare with a single treatment.
One of the most controversial points of scar surgery is when to perform the revision. There are many factors a doctor must take into consideration when looking at how to treat a scar, according to Loren Schechter, MD, FACS, chief, Division of Plastic Surgery at Chicago Medical School.
“Timing and technique may be dictated by the nature of the scar,” he says. “If, for example, the scar causes a functional problem (such as eyelid malposition leading to exposure keratitis), a revision procedure may have to be done sooner rather than later. If, however, the scar has healed uneventfully, and presents only a cosmetic concern, in general I prefer to allow the scar to mature—that is, soften, flatten, and fade prior to considering scar revision.”
During that time, scar massage, sun avoidance, and topical gel sheeting or creams may be helpful in expediting scar maturation, Schechter advises. “In adults, I tend to wait a minimum of 6 months, but ideally 9 to 12 months prior to performing a surgical scar revision. This time frame may be extended in children even up to 2 years.”
As such, he will consider surgery in specific cases when treating a scar. “I generally consider surgical scar revision if the issues are scar spreading—indentation, pincushioning, distortion of adjacent structures,” he adds. “If the issues are primarily pigment-related, camouflage makeup or laser therapy may be more appropriate.
“It is also important to counsel patients that scars do not disappear. The goal is generally to reduce the appearance of the scar or improve function. It is not to say that I won’t perform a particular procedure. It is important to tailor the procedure to the patient and the specific issues related to their scar.”


Figure 2. This patient’s laceration on the cheek was treated with two sessions of mulitpass, high-fluence, high-density CO2 laser skin resurfacing.
Joseph Niamtu III, DMD, a cosmetic surgeon in the Norfolk, Va, area, prefers to treat most scars within 8 weeks of when they occur. “Past studies of split scar treatment with chemical peel showed that the half of the scar treated within 8 weeks responded better than those treated an extended time after the event,” he states.
“Call some surgeon’s office and tell them you have a recent scar, and they will tell you to call back in a year when the scar is mature. Personally, I disagree with this. I am a believer that scars best respond to laser treatment while they are in the remodeling phase.”
Timing is also very important to David S. Kung, MD, FACS, a plastic surgeon in Washington, DC. He states, “The most important thing to do is to wait until the scar has matured. Wound healing is a process that can take 6 to 12 months to complete. In nearly all cases, scars will improve in appearance over time. Many times, a scar revision may not even be necessary.”
For those scars that do need revision, patients have to understand that a scar is permanent, Kung notes. “Once the skin is broken, there is no way to be rid of the scar. The only exception to this fact is if a scar is formed in utero. All we do as plastic surgeons is trade one scar for another. Obviously, there are techniques to change the direction, length, width, and thickness of scars. However, one must be sure that the eventual scar is better than the original.”
Robert Kotler, MD, FACS, of Beverly Hills, Calif, echoes this sentiment. “Surgical scar revision, whereby the scar is surgically removed and another effort is made at an ideal closure, is appropriate when other less invasive treatments have failed. But the surgeon runs the risk that despite the most ideal and meticulous repair, the tissues respond by forming yet another thick and unsightly scar.”
Similarly, Neil Sadick, MD, FAAD, FAACS, FACP, FACPh, a dermatologist and researcher based in Great Neck, NY, will only use surgery to fix scars in cases where the scar does not respond to laser treatment or other noninvasive applications.
For Z. Paul Lorenc, MD, FACS, a plastic surgeon in New York City, unless the scar causes a functional deficit—such as scar contracture of the lower eyelid causing exposure keratitis, or scar contracture of the oral commisure causing oral incompetence—scar revision is a last resort, and is usually performed at 12 months when the scar is mature.
Chad Tattini, MD, a cosmetic surgeon in private practice in Bloomington, Ill, adds, “I usually don’t operate until I know the scar is mature. This is usually 1 year for most parts of the body but can be up to 2 years on certain parts of the body.”
The best thing to do with a scar in high tension plains—such as the anterior chest, joints, between the shoulder blades, and from the knee down—is to leave it alone, if possible, and try conservative management, says Michael S. Kluska, DO, FAACS, FACOS, who is in private practice in Greensburg, Pa.
“The earlier the treatment, the better chance for long-term results. Every time a scar is revised, the new resultant scar will always be longer or bigger and could result in more not less scar,” notes Kluska.


Figure 3. This patient sustained a deep laceration from a fall. He is shown before and after two sessions consisting of multipass, high-fluence, highdensity laser resurfacing. Silicone oil injection is planned to elevate the depressed area.
“As a result of the above information, I try to treat the surgical scar as soon as possible. My patients all start massaging the scar with Vitamin E and Mederma, or they use one of the many other products now on the market for scar treatment,” he says.
“Finally, most physicians have been trained that scars should never be in the sun for the first year due to increased risk for redness, hypertrophy, and hyperpigmentation,” Kluska adds. “Ironically, all my patients that don’t listen and go to the tanning bed end up having the best well-hidden scars. Maybe they are onto something.”




Figure 4. This patient was treated with steroid injection, a Z-plasty, and several sessions of multipass, high-fluence, high-density CO2 laser resurfacing.
INJECTABLES AND SILICONE GEL SHEETS
Most of the physicians interviewed mention both injectables and silicone gel sheets, which are two options that can be used both before and after scar-revision therapy.
“My protocol for scar revision has evolved greatly over the last 3 years,” says Steven H. Dayan, MD, FACS, a facial plastic surgeon based in Chicago. “For hypertrophic, thickened, or keloid scars, I frequently use an intralesional injection combining 5FU, Triamcinilone 10%, and Botox in a 7-to-2-to-1 ratio. Treatment intervals are 6 to 8 weeks apart and until the scar is thin and atrophic. Any persistent erythema is then treated with IPL.
“Thickened scars and keloids are reduced to cosmetically camouflaged lesions rapidly and permanently, usually after two to three treatments. For depressed mature scars, subcision and needling with a 22-gauge needle is followed 2 weeks later by filler treatment using either thinned lidocaine, diluted Restlyane, or microdroplet silicone to efface and camouflage the scar.”
Says Samieh Sam Rizk, MD, FACS, the director at Manhattan Facial Plastic Surgery, “When I consider a scar, I think of three things: color, width, and height. Therapies should address these three qualities of a scar. If a scar is thick or has height, my first line of treatment before surgical excision is repeated Kenalog 10 injections, 3 weeks apart, and silicone sheets or cream for 6 weeks. Scarguard is excellent. If after 6 weeks I am still not happy with the height, I will consider an excision of the scar.”
The type of scar and the patient’s skin dictate the treatment of the scar, notes Michael A. Persky, MD, FACS, a facial plastic and reconstructive surgeon in Encino, Calif. “For the most part, if a scar is hypertrophic and keloided then surgical scar excision/revision is indicated. In those cases, a series of Kenalog-10 injections and silicone sheeting gel is helpful.”
“If the scar creams and lasers are not effective, then I proceed to Kenalog injections,” adds Anthony Youn, MD, a cosmetic surgeon in private practice in Rochester Hills, Mich. “Typically, I start with Kenalog 10 and warn the patient of the possibility of side effects like thinning of adjacent skin. These are performed every 4 weeks until the scar looks better.”
THE ROLE OF LASERS
For many simple surgical or traumatic scars, CO2 laser resurfacing and injectable silicone make a favorable combination, according to Niamtu. Many scars can be dramatically improved by high-fluence, high-density CO2 laser resurfacing, he adds.
“Several passes of the CO2 laser can flatten and blend scar tissue,” according to Niamtu. “Normally, several treatments spaced 90 days apart are required for optimum result. Surgical excision with geometric reapproximation is an option for many scars, but I generally end up lasering these scars, again within 8 weeks of the revision. Many scars can be improved with CO2 laser, but still have areas of depression. I have had excellent success with microinjection silicone oil to plump depressed scars.”
Regarding laser treatments, Youn uses “the Cynosure Synergy pulsed-dye laser. The laser comes into play when the scar begins to thicken and scar creams appear to not be enough. Minimally invasive and with minimal [patient] discomfort, scientific studies show that the pulsed-dye laser can visibly improve scars.”
Robert A. Shumway, MD, FACS, a cosmetic surgeon in La Jolla, Calif, tends to favor laser resurfacing when surgical scar revision is not practical or if the patient refuses surgery. “My approach to scars is to do what works for that particular scar,” he says. “How big is it? How old is it? How red or brown is it? Where is it located? Is it raised? How did you get it? How traumatic is it to the patient? There are a million questions to ask.
“Mostly, I use ablative fractional, but some people are doing nonablative fractional treatment. Additionally, for less mature scars I often resurface with Erbium-YAG full field (nonfractional), using a Sciton laser with a 2-millimeter handpiece.”



Figure 13. Following Z-plasty and placement of a composite skin graft, this nostril was stented to prevent restenosis.
Sadick, on the other hand, simply uses a pulsed-dye laser for red scars, an excimer targeted laser for white scars, and first- or second-generational fractional lasers for depressed or elevated scars.
Kotler offers the following example. “What if the scar, for whatever reason, does not flatten? It remains thickened, raised, and sometimes red. That may be the result of a less-than-ideal repair or a factor of one’s genetics. Certain ethnic groups are predisposed to thick scars—dark-skinned patients, brown or black Asian patients, American Indians, or Central and South Americans who have significant Indian genetics.
“Hypertrophic or keloid scars develop over time. They are not formed immediately, but typically 2 to 3 months after the injury or surgical incision. They can be improved by sequential injections of cortisone, and even by certain laser treatments.”
Mature ice pick, boxcar, and rolling acne scars are best treated by simultaneous combination of microdroplet fat transfer and fractionated CO2 laser resurfacing using deep and Active-FX (Lumenis Ltd, Santa Clara, Calif), according to Dayan. “Only one treatment is usually necessary to get results that are not truly realized for 6 months to 1 year,” he adds.
Robert H. Burke, MD, FACS, DDS, MS, FICS, Director of The Michigan Center for Cosmetic Surgery in Ann Arbor, uses the NLite V (ICN Pharmaceuticals, Costa Mesa, Calif) laser in flash lamp pulsed-dye mode, with a 5-mm handpiece for hyperplastic, red scars in conjunction with intralesional steroids in dealing with small keloids.
“The earliest that I use this is 8 to 12 weeks following the surgical procedure or event that led to the scar,” he says. “If the scar is postsurgical, it would have been treated with topical Scarguard or Mederma. Most of my patients start on this [treatment] 2 to 3 weeks following the procedure, after sutures are removed. If the scar is of long duration, I prefer to start with Scarguard for 3 to 6 months. If the scar is relatively fresh and red, I would start the laser therapy in conjunction with the topical.”
The use of laser-based devices can improve the color of scars if the scar is too pink or darker than surrounding skin, Rizk says. “If a scar is too wide, an excision is a better option over laser therapy.”
OTHER CONSIDERATIONS
A scar that violates the lines of skin tension will result in contractions that will improve with time but may require surgical intervention, Petro says. “Deciding whether to use a Z-plasty, a W-plasty, or local flap depends on location, size, and nature of the scar. But the core principles remain.
“Although we like to think not all incisions result in scars, no matter how carefully the surgery is performed, never promise that the scar will be invisible. [This is] whether a mole is being excised, a tattoo removed, or an incision being made for cosmetic surgery.
“Minimizing the scar is the goal according to patient selection. Avoid patients who will be unhappy with the scar no matter what. Place the incision in hidden areas, follow lines of skin tension, review in advance where the patient would like the scar, and show them some bad as well as good results.
“Then follow the patient, see them at the time when the scar will be obvious—around 6 to 12 weeks—to institute some measure of intervention, if only to show the patient that you care. Be prepared to intervene with steroid injections, laser treatment, or something to abort more aggressive, unsatisfactory scarring.”
When asked if there are any procedures or approaches that should be avoided, Sadick opines, “Microdermabrasion for scars is not helpful.”
Lorenc responded to the same question: “As far as what I won’t do, I will not perform a scar revision unless a major contributing factor to the scar changes (no tension on closure, orientation of the scar is changed, etc).”
Burke will not treat patients “with a history of multiple keloids, Ehlers-Danlos syndrome [EDS, also known as Cutis hyperelastica]; any patient who is incapable of understanding; has poor compliance, poor health, or a question of factitious scar; or has mental illness.”
“My main scar therapy for all patients is primarily daily massage and sun protection,” Tattini says. “During the early months, I also recommend taping of the scars as much as possible. Only when issues arise do I recommend the other modalities.
“I don’t recommend creams because I haven’t seen any make any difference and there are no valid human clinical studies that have proven the evidence. I certainly don’t recommend microdermabrasion because that is not aggressive enough.”
Janine Ferguson is a contributing writer for PSP. She can be reached at [email protected].