We live in an interesting time in terms of skin resurfacing. Tried and true methods, such as chemical peels, have been superceded by newer but relatively untried technologies, including fractional laser, plasma resurfacing, and other nonablative modalities.
No doubt about it: These are exciting technologies, but at the same time they disappoint. The industry and media hype surrounding the use of some devices produces a situation in which expectations—of both surgeon and patient—exceed the results. Due to this rapidly changing environment, I have seen more than one person spend over $100,000 on a laser or similar device only to be disappointed with the outcomes. The device becomes little more than an expensive door stop.
I believe I can achieve better results with $1.50 worth of trichloroacetic acid (TCA) chemical peel than thousands of dollars in laser treatments.
A HISTORY LESSON
Chemical peeling was the first skin resurfacing procedure, with reports of early civilizations using fruit acids to treat the facial skin. Aggressive chemical peeling was pervasive in Europe and was performed by lay peelers. Ethnic communities brought this art to the West Coast of the United States in the early 20th century as secret recipes with a continuation of lay treatments.
As the medical community began to observe and control chemical face peeling, the procedure was studied in numerous fashions. Aggressive phenol face peels reigned supreme for years, but these were fraught with problems, such as severe porcelain hypopigmentation, caustic burns, organ system toxicity, and death.
Over the ensuing years, phenol peeling became more controlled, but largely was displaced by TCA as the peeling agent of choice. TCA is much safer, predictable, and more easily controlled than phenol and croton oil. It is commonly used from concentrations of 15% to 70% and, although predictable, can nonetheless cause severe burns and hypopigmentation when used incorrectly.
TCA exerts its action by the almost immediate coagulation of dermal proteins, which in part through severe vasoconstriction produces a white “frost” as the coagulation proceeds. The color and intensity of the frost and skin serve as end points for various chemical peel depths, which directly correlate to healing time and clinical result.
As with all skin resurfacing procedures regardless of mechanism, chemical peeling is part art and part science, similar to dermabrasion, and less controlled than lasers. Each patient presents a unique set of circumstances that affect how the acid reacts to the skin. Skin hydration, sebum content, thickness, and actinic damage and acid concentration can all affect the penetration of acid into the dermis. Due to this, each patient may require different treatment.
Pigmented skin always presents resurfacing challenges, and chemical peeling is no exception. Although all skin types can be safely peeled with TCA, many nuances exist with pigmented skin.
The treatment of Fitzpatrick skin types 4-6 should be reserved for experienced peelers only. These patients are much more difficult to manage in terms of treatment depths, pigmentation abnormalities, and reactive skin states postpeel.
Most adult patients can be classified as having mild, moderate, or severe actinic damage, which corresponds with the same classification of dyschromias and rhytids. The novice peeler should begin with light-skinned patients with moderate dyschromias and rhytids. Although very aggressive, high-concentration TCA peels can produce dramatic laser-like results, the safety margin decreases. With like-laser skin resurfacing, it is better to seek safe moderate improvement than riskier “home runs.” The key term in any resurfacing is to be conservative.
I feel the best way to teach or learn chemical peeling is to begin with ultra-light peels on conscious patients.
UNDER THE SKIN
 |
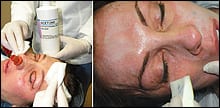
| Figure 1. Prior to acid application the face is degreased with acetone or alcohol (A, above left). The end point for light TCA chemical peels is a patchy white frost with a pink background, as shown on the forehead (B, above right). |
A 15% solution of TCA can be made by using 2 mL of 30% TCA and 2 mL of water. After degreasing the skin with acetone or alcohol (Figure 1A), a single coat of this concentration applied to the skin will induce tolerable burning and may produce very patchy areas of frost.
This level of damage would be an epidermal peel and the healing would be 2 to 3 days, usually without noticeable peeling. There is not much downtime with this level of peel, and makeup can be worn the next day. There is also no significant noticeable clinical result from a single peel at this strength. This would be considered a superficial chemical peel.
After performing this light, single-coat peel, you can proceed to multiple simultaneous coats of 15% TCA. Approximately 4 cc of this 15% mixture will cover the entire face and is applied with cotton-tipped applicators and sponges. Rub it in with gauze or simply apply it with a gloved finger.
After the entire coat is applied, then you must wait several minutes to observe the clinical signs of acid penetration before applying a second or third coat. Successive coats of 15% TCA amplify the discomfort. Don’t apply more than two coats on conscious patients.
Topical anesthesia is not used with peels, as it excessively hydrates the skin. Oral sedation and local anesthetic blocks can be used to apply three to four coats, but always utilize IV sedation when performing multiple-coat peels.
 |
| Figure 2. These images show “frost” levels of various concentrations of TCA peels: A patient immediately after three coats of 20% TCA with a moderate frost with a pink background (A); a patient after two coats of 30% TCA and figure with a dense white frost (B). |
The surgeon should slowly progress up the peel ladder and make careful observations of the healing and clinical results from one, two, and three coats of 15% TCA. Two to three coats of 15% TCA probably produce basilar epithelial damage and require 5 to 6 days to peel and re-epithelialize. The end point of this depth of peel is a white frost with a pink background (Figure 1B). Clinically, this type of peel would smooth the skin, improve epidermal melanin, and affect the finest lines and wrinkles.
TCA can be safely used in stronger concentrations by experienced peelers. A 20% mixture of TCA is made by mixing 4 mL of 30% TCA with 2 mL of water. I generally do not use more than three coats of this mixture on the face and no more than two coats on the neck. Straight 30% can also be used in a single or double coat but, again, it is reserved for experienced clinicians. The end point of this peel is a solid white frost, and it damages the skin to the papillary dermis and sometimes into the intermediate reticular dermis (IRD) (Figure 2).
This depth of injury generally is fully re-epithelialized in 1 week and the patient is back in makeup (Figure 3). Light erythema can occur for several days, but laser-like extended redness is rare.
Clinical improvement of dyschromias can be impressive at this level of peel, and fine-to-moderate skin lines can be improved. Treating the patient at 90-day intervals can make more impressive clinical results with deeper wrinkles or acne scars. I refer to a peel at this treatment level as a medium-depth chemical peel.
 |
| Figure 3. This patient is shown immediately after two coats of 30% TCA to treat lower eyelid skin wrinkling in conjunction with lower transconjunctival blepharoplasty. |
Frequently, I use a double coat of 30% TCA to treat lower-eyelid skin wrinkling in conjunction with lower transconjunctival blepharoplasty (Figure 3).
For all but the most superficial peels, patients are pretreated with retinoids and bleaching agents. This produces greater acid penetration, faster re-epithelialization, and less inflammatory hyperpigmentation problems.1-4 These patients are also treated with antivirals (Valacyclovir 500 mg BID) and with a cephalosporin antibiotic (although this remains controversial).
Some surgeons advocate highly aggressive peels using 70% TCA, but the risks, healing issues, and complications increase. I switch to laser resurfacing for these more challenging cases, which I find more accurate and predictable. More science; less art.
Postpeel care for all patients is simple and involves continual application of petrolatum or Aquaphor until the peeling is complete. The face is washed BID with fingers and using a gently hypoallergenic cleanser. Peeling begins around facial areas of greatest mobility within 2 to 3 days and is usually complete by day 7 for medium-depth peels (Figure 4).
AYE, THERE’S THE RUB
 |
| Figure 4. These patients are shown 5 days after medium-depth TCA peel and are well into the peeling phase of the recovery. Generally, the peeling is complete by day 7 with complete re-epithelialization. |
Complications of chemical peeling are similar to any resurfacing procedure and can result in overtreatment, burns, scars, hypo and hyperpigmentation, acne flair, milia, infection, and ectropian.
Safety precautions include protecting the patient from inadvertent acid exposure to other areas, especially the eyes. TCA is generally compounded in a weight/volume (W/V) manner and must be concocted by a reputable source, such as Delasco or competent local compounding pharmacies.
SOUTH OF THE EARS
The neck has less pilosebaceous units than facial skin and must be treated more conservatively. I do not use concentrations on the neck that are greater than 20% TCA—and have had some sleepless nights with that.
Unfortunately, many physicians have caused permanent scarring to the neck by overtreatment. The neck is a different animal than the face. You must respect the neck when it comes to any and all resurfacing procedures.
 |
| Figure 5. This patient is shown with UV photography before (top) and after (bottom) a single medium-depth TCA chemical peel. |
Using UV photography is an excellent means of predicting peel outcomes.4 Superficial pigmentation is enhanced by UV light, and enhancing dyschromias are likely to respond well with medium-depth peel, whereas dyschromias that do not enhance with UV light are likely deeper and may not respond as well. In addition, these scans can be used to show the surgeon and patient the degree of improvement (Figure 5).
CASE PRESENTATIONS
In three case presentations, I have basically let the photographs (Figures 6, 7, and 8) speak for themselves, except to offer a brief description.
In Figure 6, the patient is shown before and after two coats of 30% TCA for treatment of ephelides and pigmentation.
The next patient is shown before and after a single medium-depth chemical peel with three coats of 20% TCA (Figure 7).
Finally, in Figure 8 an African American patient is shown after aggressive pretreatment with Retin A and hydroquinone 4% for 8 weeks, followed by a medium-depth chemical peel.
|
|
|
CONCLUSION
Even with all the new and innovative technologies that have emerged to rejuvenate skin—including global skin—the simple TCA chemical peel remains a safe, effective, economical, and time-tested method that is adaptable to all skin types. It can produce worthy results with reasonable downtime in diverse patient populations.
Joseph Niamtu III, DMD, is a board-certified oral and maxillofacial surgeon in private practice in Richmond, Va. He can be reached at [email protected].
REFERENCES
- Obagi S, Chaudhary-Patel M. Overview of skin resurfacing modalities. In: Guthoff RF, Katowitz JA, eds. Essentials in Ophthalmology: Oculoplastics and Orbit. Berlin: Springer; 2007: 259-275.
- Obagi Z, Obagi S. Pearls for successful chemical peeling. Cosmet Dermatol. 2004; 17(6): 363-371.
- Obagi S, Bridenstine JB. Chemical skin resurfacing. Oral and Maxillofacial Surgery Clinics of North America. 2000;12(4):541-553.
- Niamtu J. Digitally processed ultraviolet images: a convenient, affordable, reproducible means of illustrating ultraviolet clinical examination. Dermatol Surg. 2001;27(12):1039-1042