Hard and soft tissue changes from trauma, developmental deformities, and surgery present unique demands for reconstruction.
Many choices are available, including lifting procedures, injectable fat and fillers, and implant reconstruction.
Although facial implants are most commonly associated with aesthetic rejuvenation, they can be extremely useful for reconstructive purposes.
The role of facial implants is to provide augmentation and volume to aging or deficient tissues, which also makes them useful in reconstructive applications.
Custom CAD-CAM implants have been a welcome innovation for both aesthetic and reconstructive patients. This technology allows precise reconstruction of defects from trauma or surgery, giving the surgeon (and the patient, in some cases) more input and control of the augmentation of prosthesis.
This article details several cases that show how facial implants can assist in reconstructive cases.
 |
 |
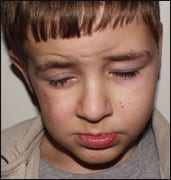
| Figure 1. An 8-year-old patient with a postradiation facial defect. | Figure 2. This CT-generated, custom skeletal model reflects the young patient’s hard-tissue changes and defects. |
CASE 1
The male patient pictured in Figure 1 was diagnosed with a rhabdomyosarcoma of the right orbit in infancy. He was successfully treated with radiation, but that process left him blind in his right eye. In addition, radiation stunted further facial growth on the affected side.
His temporomandibular joint became hypoplastic and ankylotic, which impeded normal mandibular growth.
The teeth buds were severely damaged, and his maxilla and midface did not properly develop on the radiated side.
In addition, he has a temporal deficiency. A computer-generated model shows the patient’s skeletal deficiencies (Figure 2).
Of the many reconstructive conundrums encountered in this case, the patient’s age and the fact that he had at least 1 decade of facial growth made definitive reconstruction difficult.
In addition, due to the highly irradiated tissues, midface and mandibular osteotomies and orthodontics were complicated.
The patient had been treated over the years with temporary solutions, including facial fillers and fat injections.
The master plan was to construct customized computer-generated implants when his growth was complete, and to consider facial bone osteotomies.
As the patient entered puberty, he became more self-conscious of his appearance. His parents requested intermediary treatment to improve his appearance.
Continued treatment with lipotransfer resulted in some improvements, but fat retention was problematic.
Resorbable and permanent facial fillers were used to make small improvements. As the patient has not completed his facial growth, a temporary solution was reached by using a pair of stock silicone submalar implants to augment his hypoplastic midface (Figure 3).
 |
| Figure 3. The left image shows how a large implant was inverted to match the contour of the defect. The center images show two implants stacked, and the right image shows the implants in situ. |
Two implants were stacked and connected with permanent suture.
A routine midface subperiosteal dissection was performed. The dissection was tenuous, as the radiated tissues were very adherent.
The stacked implants were inserted in the dissection pocket, producing an improved contour of the right face (Figure 4).
 |
| Figure 4. The patient is shown before and after stacked implant placement in the right midface. |
This noncustom augmentation has remained stable and without problems for more than 3 years.
The patient was quite pleased with the temporary solution, and when his facial growth is completed a more complex series of custom implants in the temporal, malar, and anterior maxillary regions are anticipated.
CASE 2
This female patient has significant manifestations from rheumatoid arthritis (Figure 5).
 |
| Figure 5. The patient is shown with the significant manifestations from rheumatoid arthritis. |
Her problems included arthritic deformities of the hands and face. The patient had severe resorption of the TMJs, which produced a severe mandibular retrognathia, loss of mandibular angle definition, accentuation of submental fat, and a midline shift of the chin.
Although this case would be an excellent one for CAD-CAM custom implants, the patient did not desire the expense and was treated with multiple off-the-shelf silicone implants.
Mandibular angle implants were placed to reproduce normal mandibular contours (Figure 6).
Submental liposuction was performed in order to improve the neck, and a silicone extended anatomic chin implant was placed.
 |
 |
| Figure 6. A silicone mandibular angle implant is shown. Note that it is held in place with a fixation screw. | Figure 7. A silicone chin implant was placed with the midline intentionally shifted to compensate for the chin asymmetry. |
This implant was placed off-center to even her chin asymmetry from the shifted mandible (Figure 7).
A unilateral submalar implant was placed to correct the hypoplastic left cheek, at the patient’s request.
 |
 |
| Figure 8. The patient is shown before and after reconstruction of multiple facial asymmetries with silicone implants. Note the improvement of her chin and submental aesthetics, as well as the improved aesthetics in the mandibular angle region. | Figure 9. Another view of the same patient, reflecting the chin and neck changes as well as the improved symmetry of the left submalar region. |
Figures 8 and 9 show the improvement of the patient after implant reconstruction of the mandibular angles, chin, and left submalar region, with combined submental liposuction.
CASE 3
This patient presented with significant lipo atrophy from antiretroviral medication.
He was treated with extralarge combined submalar shell silicone implants to restore facial contours (Figures 10 and 11).
 |
 |
| Figure 10. Frontal before-and-after images show the improvement of the severely atrophic midface. | Figure 11. An oblique view is shown of the same patient. |
 |
| Figure 12. This panoramic radiograph shows the resorptive defects; and a picture of the patient illustrates the corresponding soft-tissue defect. |
CASE 4
This patient underwent maxillary and mandibular osteotomy—with severe bilateral idiopathic bone resorption manifested by defects in the mandibular border (Figure 12).
This left a significant deformity that was difficult to correct.
A mandibular model was constructed from a CT scan, after which bilateral, porous polyethylene custom implants were constructed (Figure 13).
The implants were contoured to fit the inferior mandibular border like a saddle on a horse.
Restoring the mandibular border corrected the soft-tissue component of the defects (Figure 14).
 |
| Figure 13. The computer-generated mandibular model is shown with the custom implants in place. |
 |
| Figure 14. This shows the patient 3 years after the reconstruction, with a totally corrected and aesthetic result. |
CASE 5
A patient presented to the office after having a horizontal osteotomy of the chin earlier in life.
She had bone resorption bilaterally in the mandibular parasymhyseal regions.
 |
| Figure 15. In order to correct resorptive defects lateral to the chin, a chin implant was positioned and the center of the implant was then removed. The remaining implant wings were then secured with fixation micro screws. |
|
See also “It Takes a Team” by Rich Smith in the April 2007 issue of PSP. |
A silicone chin implant was placed. The center of the implant was removed so that only the depressed regions were augmented (Figure 15).
DISCUSSION
Reconstruction of hard- and soft-tissue defects present many challenges and are amenable to many forms of therapy.
Standard and computer-generated customized implants can be useful adjuncts in many cases.
Joseph P. Niamtu III, DMD, is a board-certified oral and maxillofacial surgeon in private practice in Richmond, Va. He can be reached at .