|
 |
 |
 |
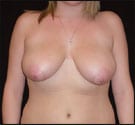
| Figure 1. A 26-year-old female before and 2 months after bilateral breast reduction using Quill barbed suture. Use of this suture allows the surgeon to perform meticulous, precise wound edge approximation. | |
With health care rising and an increasingly competitive aesthetic medicine industry, today’s surgeon must invent ways to be more efficient in order to meet the demands of the marketplace.
One of the easiest ways to accomplish this is by being able to perform complex surgeries more quickly and efficiently, therefore allowing the surgeon to service more patients.
An example of a technology that can help you make the complex procedure simpler is the barbed suture.
Available in both absorbable and non-absorbable materials, Quill double-armed sutures (from Angiotech Pharmaceuticals Inc, Vancouver, British Columbia, Canada) allow for rapid bidirectional wound closure without the use of multiple, individual stitches.
The barbed suture allows for excellent deep tissue and subcuticular wound-edge approximation and does away with knot tying.
Via micromachining techniques, the bidirectional wound closure device is fabricated from monofilament fibers combined with etching of the filament in order to create barbs in a helical fashion.
Furthermore, the barbs vary in lengths and oppose one another from the midpoint of the suture length (Figure 1).
This configuration ultimately allows for a linear “drawstring” closure of the wound. This type of closure translates into a well-approximated wound at multiple tissue levels, with a decrease in tension in the X, Y, and Z axis.
THE ADVANTAGES
Use of the barbed suture has multiple advantages over the traditional wound-closure devices.
First and foremost, the barbed suture allows for rapid, consistent closure of the wound. As the suture holds tension on its own, the need for knot tying has been eliminated, thereby decreasing surgeon fatigue.
In addition, it is a known fact that every interrupted stitch that is placed into a wound edge results in small areas of edema and ischemic changes around the stitch, showing microscopic diminished blood supply.
When you use a barbed suture that does not require knots, the wound edge inherently receives an improved blood supply. This translates into better wound-edge approximation, with increased vascular supply and, ultimately, better cosmesis.
As the suture is a running, continuous stitch, less suture material is needed, which results in a dollar-cost savings for the surgical facility as well. An example of this can be seen in the traditional breast-reduction patient.
Anecdotally, it was the use of the barbed suture in my surgical cases that has helped to decrease my operatory time by as much as 20 minutes per breast-reduction case. Overall, I have realized an average cost savings of between $100 and $150 per case.
The Disadvantages
Were one to look for a drawback to the barbed suture, it would be a technical issue: As the suture is barbed, it cannot be laid down on the surgical drapes due to risk of snagging. This could result in a suture that becomes imbedded into the drapes and unusable.
For similar reasons, the surgeon must be cautious when he or she wipes or dabs the wound edge while closing. Again, the gauze in the wipe could get caught in the barbs, which could result in fibers being imbedded into the suture as well as a loss of integrity to the individual barb. Ultimately, this could lead to a decrease in integrity of the continuous suture.
Another potential problem associated with any continuous stitch is the potential for breakage. If this were to occur, the surgeon would have two options: remove the stitch completely or cut it in front of the break point and then start a new barbed suture at that point.
Finally, if the surgeon places the stitch in a plane or location not to his or her liking, the stitch cannot be reversed or pulled through due to the barbs.
USING THE BARBED SUTURE
In order to maximize the efficiency of this product, the surgeon must master a few technical caveats associated with its use.
For example, when placing this suture, the surgeon must follow a simple four-step process.
First, lightly stretch it while under gentle traction. This not only diminishes the memory but also activates or “sets” the barbs by springing them open to their maximum potential.
|
See also “Treating the Aging Neck,” by Malcolm D. Paul, MD, FACS, in the November 2007 issue of PSP. |
Second, the surgeon should place a completely stretched-out suture just above the wound edge in order to roughly “measure” the wound. This will allow the physician to ensure adequate length and, therefore, decrease the opening of multiple sutures of inappropriate length.
Third, after the stitch is placed, it must be gently pulled to its center point. In doing so, the surgeon will feel where the suture catches with resistance. A good safety check for this would be to tent up both ends of the suture, making sure that each arm is of equal length.
Fourth, it is important for the surgeon to maintain placement of the suture in the same horizontal plane. This allows for meticulous, precise wound edge approximation (Figure 1).
As one can see, the disadvantages are somewhat similar to those of many of the surgical products that we use. Any problems are easily preventable once you have learned how to use the product.
Michael S. Kluska, DO, FAACS, FACOS, is a dual board-certified plastic and reconstructive surgeon and general surgeon in private practice in Greensburg, Pa. He is a graduate of Washington & Jefferson College with an undergraduate degree in art. He attended medical school at Des Moines University. Kluska can be reached at .